Beating Nausea
Nausea and vomiting are less common side effects of chemotherapy today, thanks to newer drugs that don't cause this problem. Some chemotherapy regimens, like oral "CMF", Taxol and Taxotere cause very little nausea at all, while others, like "AC" cause moderate nausea in about one-third of patients.
When the nausea does occur, it is only occasionally associated with actual vomiting, and it may occur some days after the chemotherapy, rather than immediately. With “AC”, for example, it is quite common to feel perfectly OK for 4-5 days, then to have a couple of “ordinary” days, where you feel low-grade nausea, rather like morning sickness. This often lifts suddenly and completely on about the 7th day. Commonly the final week before the next course of chemotherapy is free of problems altogether.
It is exceedingly uncommon these days for patients to be bed-bound by their nausea, or to require hospital admission
Minimising Nausea
The mainstay of preventing chemotherapy-related nausea is the use of potent anti-nausea drugs. These are known as “anti-emetics”. You will be administered some anti-emetics intravenously at the time of your chemotherapy by the chemotherapy nurse. Others will be prescribed for you to take orally. It is critically important that you take these exactly as prescribed and not try to “cut corners” by leaving some out.
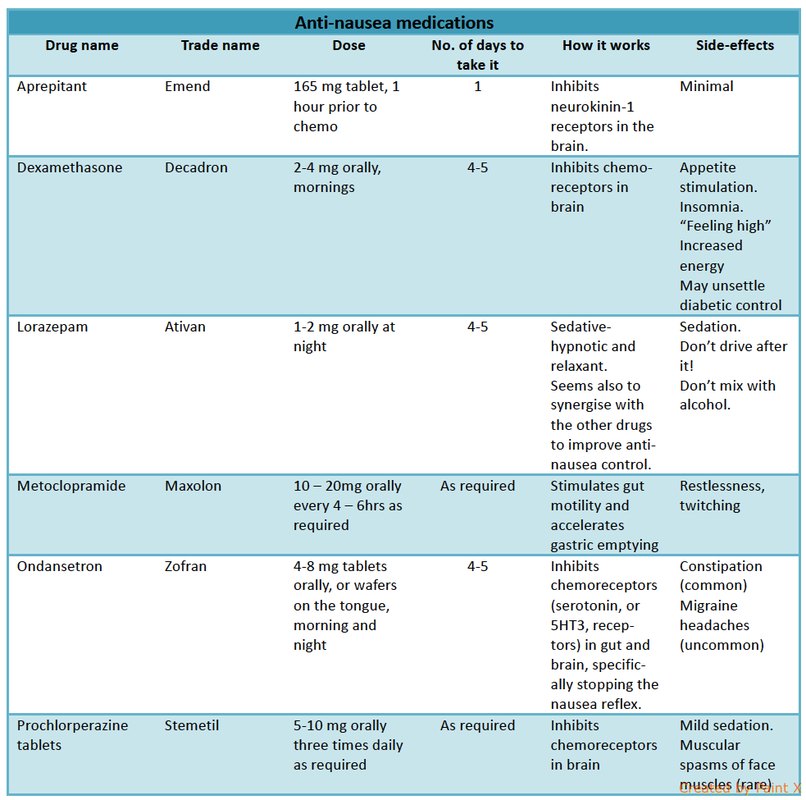
I will be prescribing a number of anti-nausea drugs for you. Details concerning them are shown in the Table.
When the nausea does occur, it is only occasionally associated with actual vomiting, and it may occur some days after the chemotherapy, rather than immediately. With “AC”, for example, it is quite common to feel perfectly OK for 4-5 days, then to have a couple of “ordinary” days, where you feel low-grade nausea, rather like morning sickness. This often lifts suddenly and completely on about the 7th day. Commonly the final week before the next course of chemotherapy is free of problems altogether.
It is exceedingly uncommon these days for patients to be bed-bound by their nausea, or to require hospital admission
Minimising Nausea
The mainstay of preventing chemotherapy-related nausea is the use of potent anti-nausea drugs. These are known as “anti-emetics”. You will be administered some anti-emetics intravenously at the time of your chemotherapy by the chemotherapy nurse. Others will be prescribed for you to take orally. It is critically important that you take these exactly as prescribed and not try to “cut corners” by leaving some out.
I will be prescribing a number of anti-nausea drugs for you. Details concerning them are shown in the Table.
Note that Zofran often causes constipation and that can make nausea worse! Not everyone gets the constipation, but I advise you to keep up the prune juice and plenty of fresh fruit and veges. You will have some Coloxyl and Senna tablets and Macrogol sachets on hand.
Tips on what to do if you're nauseated.
Tips on what to do if you're nauseated.
- Eat small, frequent meals throughout the day instead of three large meals. (Nausea is often worse if your stomach is empty).
- Eat slowly, chew your food completely and try to stay relaxed.
- Eat foods that are cold or are at room temperature. (The smell of hot or warm foods may make you more nauseous).
- Try to avoid preparing food – get the family to do it, and only come to the kitchen or dining area when it is on the table.
- Avoid eating foods that are hard to digest such as spicy foods or foods that are high in fat (including rich and creamy sauces).
- Rest after eating. If you need to lie down, keep your head elevated on a couple of pillows.
- If you feel nauseated when you first wake up, try keeping a box of dry biscuits next to the bed and eat a few, ideally with a cup of black tea, before getting out of bed. Or, try eating a high-protein snack such as lean meat or cheese before going to bed (protein takes longer to digest).
- Instead of drinking beverages with your meals, drink beverages and other fluids between meals.
- Drink six to eight middy glasses of fluid (preferably water) per day to prevent dehydration. Choose cold beverages such as flat soda or flavored drink mixes. You can also choose ice cubes, or ice-blocks.
- Try to eat more food at a time of the day when you feel less nauseated.
- If you have been feeling nauseated, be sure to tell your chemotherapy nurse before each treatment session and mention it to the doctor at your appointment.
- Contact the chemotherapy clinic or my nurse if your nausea causes vomiting that is persistent or severe (if you can't keep fluids or foods down on a continual basis). Persistent vomiting can cause dehydration and should be treated immediately. Occasionally this requires a brief period on a drip. This always settles things down very quickly, but it is VERY RARELY NECESSARY.
- Take your Stemetil (Prochloperazine) or Maxolon (Metoclopramide) 1/2 hour to 1 hour before eating.